TMJ Guide
Carpal Tunnel Surgery: Is It Worth It? (What to Expect)
Carpal tunnel relief guide.
By Expert Team · Published 2026-03-10 · Updated 2026-03-10
Carpal tunnel surgery is a common outpatient procedure with a success rate above 90%, designed to relieve pressure on the median nerve by cutting the transverse carpal ligament. Most patients experience significant pain relief within weeks, regain full hand strength by 6 to 12 weeks, and report lasting improvement in numbness, tingling, and grip strength for years after the operation.
By Dr. Laura Chen, Occupational Therapist & RSI Specialist Last updated: March 2026
Table of Contents
- When Is Carpal Tunnel Surgery Recommended?
- Open vs Endoscopic Carpal Tunnel Surgery
- What Happens During Carpal Tunnel Surgery
- Recovery Timeline: Day 1 to 12 Weeks
- Success Rates and Long-Term Outcomes
- Risks and Potential Complications
- How Much Does Carpal Tunnel Surgery Cost?
- Surgery vs Conservative Treatment
- Preparing for Carpal Tunnel Surgery
- Post-Surgery Rehabilitation and Exercises
- Frequently Asked Questions
- Sources
When Is Carpal Tunnel Surgery Recommended?
Carpal tunnel surgery — formally called carpal tunnel release (CTR) — is not usually the first line of treatment. Your doctor will typically recommend surgery when conservative approaches have failed to provide adequate relief over a period of several weeks to months.
Specific indications for surgery include:
- Persistent symptoms lasting more than 6 months despite splinting, corticosteroid injections, and activity modification
- Moderate to severe nerve conduction study results confirming significant median nerve compression
- Thenar muscle atrophy — visible wasting of the muscles at the base of the thumb
- Constant numbness or tingling in the thumb, index, middle, and ring fingers that does not respond to a wrist brace
- Severe pain that disrupts sleep, work, or daily activities
- Acute carpal tunnel syndrome caused by trauma such as a wrist fracture
If you are still in the early stages of carpal tunnel syndrome and have not yet tried conservative options, you may want to start with targeted carpal tunnel exercises before considering surgery. Many mild cases respond well to non-surgical management.
It is worth noting that delaying surgery when nerve damage is progressing can lead to permanent sensory loss and muscle weakness. If your hand surgeon recommends surgery, the evidence strongly supports acting sooner rather than later.
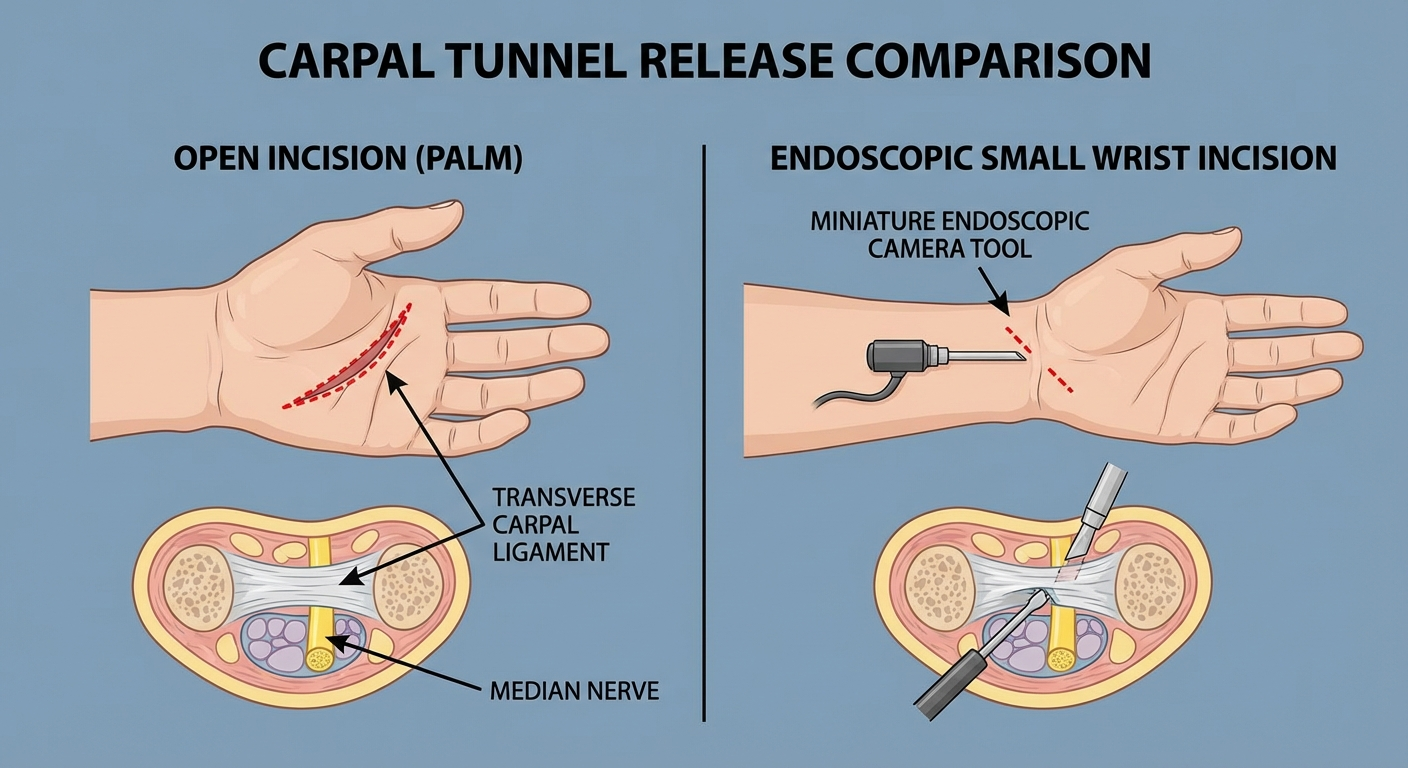
Open vs Endoscopic Carpal Tunnel Surgery
There are two primary surgical techniques for carpal tunnel release. Both accomplish the same goal — dividing the transverse carpal ligament to decompress the median nerve — but they differ in approach, incision size, and recovery characteristics.
Comparison Table: Open vs Endoscopic Carpal Tunnel Release
| Feature | Open Release | Endoscopic Release |
|---|---|---|
| Incision size | 2–3 cm in the palm | 1–2 small incisions (wrist/palm) |
| Anesthesia | Local or regional | Local or regional |
| Procedure time | 15–30 minutes | 15–30 minutes |
| Visualization | Direct view of the ligament | Camera-guided via endoscope |
| Pillar pain | More common | Less common |
| Return to light work | 2–4 weeks | 1–3 weeks |
| Return to heavy labor | 6–8 weeks | 4–6 weeks |
| Grip strength recovery | Slightly slower | Slightly faster |
| Success rate | 90–95% | 90–95% |
| Scar size | Larger, palm-based | Smaller, wrist-based |
| Risk of nerve injury | Very low | Slightly higher (rare) |
| Cost | Generally lower | Generally higher |
| Surgeon experience needed | Standard | Specialized training required |
Open Carpal Tunnel Release
Open release is the traditional and most widely performed method. The surgeon makes a single incision of approximately 2 to 3 centimeters along the base of the palm, directly over the carpal tunnel. This provides a clear, direct view of the transverse carpal ligament, which is then carefully divided under direct visualization.
Advantages: The open approach gives the surgeon full visibility of the anatomy, reducing the risk of inadvertent nerve or artery damage. It requires no specialized endoscopic equipment, is available at virtually every surgical center, and has decades of outcome data supporting its effectiveness.
Disadvantages: The palm incision can cause what is known as "pillar pain" — tenderness at the base of the palm where the incision was made. Recovery of grip strength may take slightly longer compared to the endoscopic approach.
Endoscopic Carpal Tunnel Release
Endoscopic release uses one or two small incisions (typically at the wrist crease, and sometimes a second at the palm) through which a thin tube with a camera (endoscope) and a small blade are inserted. The surgeon visualizes the ligament on a monitor and divides it from the underside.
Advantages: Smaller incisions generally mean less postoperative pain, faster grip strength recovery, and an earlier return to work — particularly manual labor. Scarring is minimal and usually well-hidden at the wrist crease.
Disadvantages: The limited field of view carries a slightly elevated (though still very low) risk of incomplete ligament release or injury to nearby structures. The procedure requires specialized equipment and a surgeon trained in the technique.
Which Should You Choose?
For most patients, outcomes are equivalent at the 3-month mark and beyond. The choice often comes down to your surgeon's experience and preference. If rapid return to manual work is a priority, endoscopic release may offer a modest advantage. If your anatomy is complex or you have had previous wrist surgery, your surgeon may recommend the open approach for safety.
What Happens During Carpal Tunnel Surgery
Understanding the step-by-step process can reduce anxiety and help you prepare.
Before the Procedure
- You will meet with your surgeon to review your nerve conduction study results and discuss the surgical plan.
- Blood tests and a basic health screening may be required, especially if you have diabetes or other chronic conditions.
- You will be asked to stop blood-thinning medications (such as aspirin or ibuprofen) several days before surgery.
- The procedure is almost always performed on an outpatient basis — you go home the same day.
During the Procedure
- Anesthesia: Most carpal tunnel surgeries use local anesthesia (injected into the wrist and hand) with optional light sedation. General anesthesia is rarely needed.
- Tourniquet: A tourniquet is placed on the upper arm to minimize bleeding and improve visibility.
- Incision: The surgeon makes the incision (palm for open, wrist for endoscopic).
- Ligament division: The transverse carpal ligament is carefully cut along its full length, immediately relieving pressure on the median nerve.
- Inspection: The surgeon inspects the median nerve for any signs of damage, scarring, or other abnormalities.
- Closure: The skin is closed with sutures or adhesive strips. The ligament is left divided — over time, scar tissue fills the gap, creating a longer tunnel with more room for the nerve.
- Bandaging: A bulky dressing and sometimes a wrist splint are applied.
The entire procedure typically takes 15 to 30 minutes.
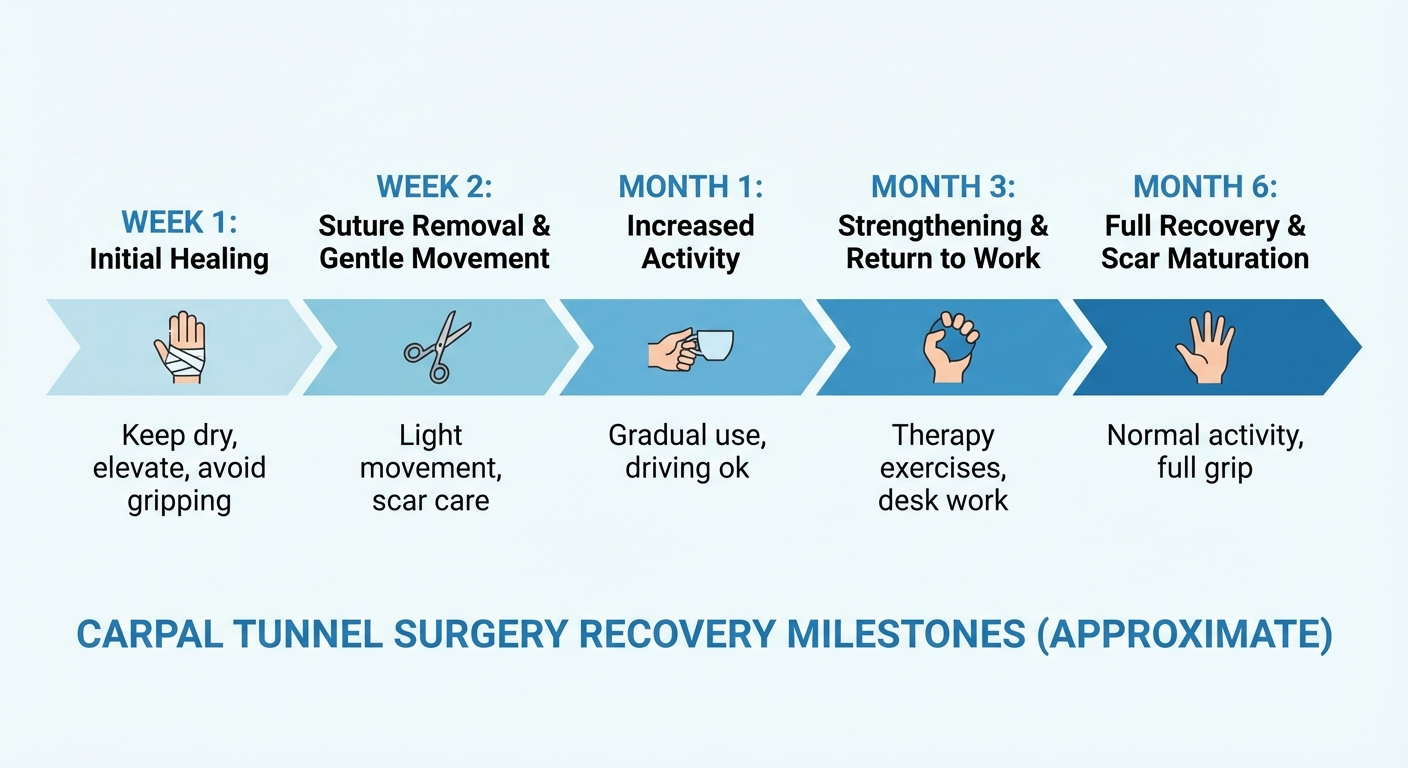
Recovery Timeline: Day 1 to 12 Weeks
Recovery from carpal tunnel surgery follows a fairly predictable pattern, though individual experiences vary based on the severity of pre-surgical nerve damage, the surgical technique used, and your overall health.
Week 1: Immediate Post-Operative Phase
- Day 1: Expect moderate soreness once the local anesthesia wears off. Keep the hand elevated above heart level as much as possible to control swelling. Move your fingers gently — this is encouraged from day one.
- Days 2–3: Pain is typically manageable with over-the-counter acetaminophen or prescription pain medication if needed. Many patients notice that their pre-surgical numbness and tingling has already improved.
- Days 5–7: The bulky dressing is usually removed, and a lighter bandage is applied. You can typically shower with a waterproof covering over the hand.
Weeks 2–3: Early Recovery
- Sutures are removed (if non-dissolvable sutures were used), usually around day 10 to 14.
- Light activities such as eating, writing, and using a phone are generally comfortable.
- Avoid gripping, lifting, or twisting motions with the affected hand.
- Scar management with gentle massage may begin once the incision has fully closed.
Weeks 4–6: Progressive Strengthening
- Most patients can return to desk work and light duties.
- Grip strength begins to return but is often still reduced compared to your unaffected hand.
- Your surgeon or occupational therapist may prescribe a structured exercise program to restore range of motion and strength.
- Pillar pain (tenderness at the incision site) is common and gradually resolves.
Weeks 6–12: Full Recovery
- The majority of patients regain full or near-full grip strength.
- Return to heavy manual labor, sports, and unrestricted activities is typically cleared around weeks 8 to 12.
- Scar tissue continues to mature and soften for up to 6 months.
- Any residual numbness from pre-surgical nerve damage may continue to improve gradually over 6 to 12 months.
Success Rates and Long-Term Outcomes
Carpal tunnel surgery has one of the highest success rates of any orthopedic procedure. Here is what the research shows:
- Symptom relief: Over 90% of patients report significant or complete relief of numbness, tingling, and pain following surgery.
- Long-term durability: Studies with 10+ year follow-up show that the vast majority of patients maintain their improvement. Recurrence rates are estimated at 1–5%.
- Night symptoms: Night-time numbness and waking due to hand pain — among the most bothersome symptoms of carpal tunnel syndrome — resolve in the majority of patients within the first few weeks.
- Grip strength: Most patients regain full grip and pinch strength within 3 to 6 months, though this depends on the degree of pre-surgical muscle wasting.
- Patient satisfaction: Large outcome studies consistently report satisfaction rates above 85–90%.
Factors That Influence Outcomes
Several factors affect how well you will recover:
- Duration of symptoms before surgery: Patients who undergo surgery before severe nerve damage occurs tend to have better outcomes.
- Severity of nerve damage: Those with significant thenar atrophy or constant numbness may not fully recover sensation or muscle bulk, even with successful surgery.
- Age: Older patients may recover more slowly but still experience meaningful symptom relief.
- Underlying conditions: Diabetes, rheumatoid arthritis, and thyroid disorders can affect nerve healing and recovery speed.
- Bilateral involvement: If both hands are affected, surgeons typically operate on the more symptomatic hand first, with the second surgery scheduled 4 to 8 weeks later.
Risks and Potential Complications
While carpal tunnel surgery is considered safe, all surgical procedures carry some degree of risk. Potential complications include:
- Infection: Occurs in fewer than 1% of cases. Signs include increasing redness, swelling, warmth, and drainage from the incision.
- Nerve or artery injury: Extremely rare (less than 0.5%) but can cause permanent numbness, weakness, or chronic pain.
- Pillar pain: Tenderness at the base of the palm near the incision site, reported by 10–30% of patients. It typically resolves within 2 to 4 months.
- Incomplete release: The ligament may not be fully divided, leading to persistent symptoms. This is more common with endoscopic approaches but still rare.
- Scar tenderness or hypertrophic scarring: Some patients develop a thickened, sensitive scar that requires ongoing massage or, rarely, scar revision.
- Complex regional pain syndrome (CRPS): A rare but serious complication causing disproportionate pain, swelling, and skin changes. Incidence is well under 1%.
- Recurrence: Symptoms return in 1–5% of patients, sometimes requiring revision surgery.
- Stiffness: Temporary finger stiffness can occur if the hand is not mobilized early after surgery.
It is important to discuss these risks with your surgeon and weigh them against the potential benefits — particularly if your symptoms are severe and progressive.
How Much Does Carpal Tunnel Surgery Cost?
The cost of carpal tunnel surgery varies significantly based on your location, insurance coverage, surgical technique, and facility type.
Typical Cost Ranges (United States, 2025–2026)
| Cost Component | Estimated Range |
|---|---|
| Surgeon's fee | $1,500–$4,000 |
| Facility/operating room fee | $1,000–$5,000 |
| Anesthesia | $500–$1,500 |
| Pre-surgical testing | $200–$500 |
| Post-surgical visits | $200–$600 |
| Total without insurance | $3,000–$10,000+ |
| Total with insurance | $500–$2,500 (copay/deductible) |
Most private insurance plans and Medicare cover carpal tunnel surgery when it is deemed medically necessary — which it usually is when conservative treatment has failed and nerve conduction studies confirm the diagnosis.
Ways to Manage Costs
- Verify your insurance coverage and pre-authorization requirements before scheduling.
- Ask your surgeon about ambulatory surgery centers (ASCs), which are often significantly cheaper than hospital operating rooms.
- Inquire about bundled pricing that includes all fees in a single quote.
- If uninsured, ask about cash-pay discounts — many facilities offer reduced rates for self-pay patients.
Post-Surgery Supplies
You may need a few items for a comfortable recovery at home:
Shop Wrist Splints for Post-Surgery Recovery on Amazon
Shop Cold Therapy Wraps for Hand and Wrist on Amazon
Surgery vs Conservative Treatment
One of the most common questions patients ask is whether they truly need surgery or whether conservative treatment could still work. Here is how to think about it.
When Conservative Treatment May Be Sufficient
- Symptoms are mild to moderate and have been present for less than 6 months.
- Nerve conduction studies show mild compression.
- Night splinting, activity modification, and corticosteroid injections provide meaningful relief.
- There is no evidence of thenar muscle wasting.
If you have not yet tried a dedicated wrist brace, a properly fitted carpal tunnel brace worn at night can significantly reduce symptoms in mild cases.
When Surgery Is the Better Choice
- Conservative measures have been tried for 3 to 6 months without adequate improvement.
- Symptoms are worsening despite treatment.
- Nerve conduction studies show moderate to severe compression.
- There is visible muscle wasting or constant numbness.
- Pain and dysfunction significantly affect quality of life.
Head-to-Head Evidence
A landmark randomized controlled trial published in JAMA compared surgery to splinting in patients with moderate carpal tunnel syndrome. At 18 months, 90% of the surgery group had successful outcomes versus 75% of the splinting group. Notably, 41% of patients in the splinting group eventually crossed over to surgery because their symptoms did not improve enough.
This suggests that while conservative treatment is a reasonable first step, surgery offers more reliable and durable relief for patients with moderate to severe disease.
It is also important to ensure your symptoms are correctly diagnosed. Conditions like tendonitis can mimic carpal tunnel syndrome, and treating the wrong condition will not help.
Preparing for Carpal Tunnel Surgery
Proper preparation can make your surgery and recovery smoother.
Medical Preparation
- Complete all pre-operative testing (blood work, nerve conduction studies) as directed.
- Disclose all medications and supplements to your surgeon, including over-the-counter products.
- Stop blood thinners as directed — typically 5 to 7 days before surgery for aspirin, 1 to 2 days for NSAIDs like ibuprofen.
- Arrange transportation — you will not be able to drive yourself home.
- Plan for time off work — typically 1 to 2 weeks for desk work, 4 to 8 weeks for manual labor.
Home Preparation
- Prepare meals in advance or arrange for help with cooking during the first week.
- Set up a comfortable recovery space with your hand elevated.
- Have loose-fitting, button-front clothing ready (pulling shirts over your head will be difficult).
- Stock up on recovery supplies:
Shop Post-Surgery Hand Recovery Kits on Amazon
Post-Surgery Rehabilitation and Exercises
Rehabilitation is a critical and often underappreciated part of the recovery process. A structured rehab program can accelerate your return to full function and minimize complications like stiffness and scar adhesion.
Phase 1: Immediate Post-Op (Weeks 1–2)
- Finger tendon gliding exercises: Gently move through fist, hook, tabletop, and straight positions to prevent tendon adhesions.
- Finger opposition: Lightly touch each fingertip to the thumb.
- Elevation: Keep the hand above heart level when resting.
Phase 2: Early Mobilization (Weeks 2–4)
- Wrist range of motion: Gentle flexion, extension, and radial/ulnar deviation.
- Scar massage: Once the incision is fully closed, massage the scar with lotion using firm, circular pressure for 5 minutes, 2 to 3 times daily.
- Light functional activities: Begin using the hand for self-care, eating, and writing.
Phase 3: Strengthening (Weeks 4–8)
- Grip strengthening: Use a soft therapy ball or putty, gradually increasing resistance.
- Pinch strengthening: Practice tip, lateral, and palmar pinch exercises.
- Progressive return to work tasks: Gradually reintroduce typing, tool use, and lifting.
For a full library of exercises tailored to carpal tunnel recovery, see our detailed guide on carpal tunnel exercises.
Phase 4: Full Return (Weeks 8–12)
- Unrestricted activity as tolerated.
- Continue strengthening exercises 3 to 4 times per week for maintenance.
- Address any residual stiffness or weakness with your occupational therapist.
Frequently Asked Questions
How painful is carpal tunnel surgery?
Most patients describe the pain as moderate and manageable. During the procedure, local anesthesia keeps you comfortable — you may feel pressure but not sharp pain. Post-operatively, soreness peaks within the first 48 hours and is typically controlled with over-the-counter pain medication like acetaminophen. By the end of the first week, most patients require little to no pain medication.
How long does carpal tunnel surgery take?
The procedure itself takes approximately 15 to 30 minutes. However, plan for a total time at the surgical facility of 2 to 3 hours, which includes pre-operative preparation, the surgery itself, and a brief recovery period before discharge.
Can carpal tunnel come back after surgery?
Recurrence is uncommon, occurring in an estimated 1 to 5 percent of patients. When symptoms do return, they may be caused by scar tissue formation around the nerve, incomplete ligament release, or progression of an underlying condition. Revision surgery is available if needed but is rarely required.
When can I drive after carpal tunnel surgery?
Most patients can resume driving within 1 to 2 weeks, once they can comfortably grip the steering wheel and operate the vehicle controls without pain. Your surgeon will provide specific guidance based on your recovery. For safety, do not drive while taking prescription pain medication.
When can I return to work after carpal tunnel surgery?
This depends on your occupation. Desk workers can often return within 1 to 3 weeks. Those in jobs requiring moderate hand use may need 3 to 4 weeks. Heavy manual laborers typically require 6 to 8 weeks before full return. Your surgeon and occupational therapist can help create a graduated return-to-work plan.
Is carpal tunnel surgery covered by insurance?
Yes, most private insurance plans and Medicare cover carpal tunnel surgery when it is medically necessary. This typically requires documentation of failed conservative treatment and confirmatory nerve conduction study results. Contact your insurance provider to verify coverage and any pre-authorization requirements.
What is the difference between open and endoscopic carpal tunnel surgery?
Open surgery uses a single 2–3 cm incision in the palm to directly visualize and cut the transverse carpal ligament. Endoscopic surgery uses one or two smaller incisions at the wrist through which a camera and blade are inserted. Both have equivalent long-term success rates above 90%, but endoscopic surgery may offer a slightly faster return to work and less palm tenderness.
Sources
- American Academy of Orthopaedic Surgeons (AAOS). "Carpal Tunnel Syndrome — Surgical Treatment." OrthoInfo, 2024. https://orthoinfo.aaos.org
- Gerritsen, A.A.M., et al. "Splinting vs Surgery for the Treatment of Carpal Tunnel Syndrome: A Randomized Controlled Trial." JAMA, vol. 288, no. 10, 2002, pp. 1245–1251.
- Atroshi, I., et al. "Outcomes of Endoscopic Surgery Compared with Open Surgery for Carpal Tunnel Syndrome Among Employed Patients." BMJ, vol. 332, 2006, pp. 1473.
- Huisstede, B.M., et al. "Carpal Tunnel Syndrome: Effectiveness of Surgical and Nonsurgical Treatment — A Systematic Review." Archives of Physical Medicine and Rehabilitation, vol. 91, no. 7, 2010, pp. 981–1004.
- Verdugo, R.J., et al. "Surgical versus Non-Surgical Treatment for Carpal Tunnel Syndrome." Cochrane Database of Systematic Reviews, 2008.
- American Society for Surgery of the Hand (ASSH). "Carpal Tunnel Syndrome." HandCare, 2024. https://www.assh.org
- Scholten, R.J., et al. "Surgical Treatment Options for Carpal Tunnel Syndrome." Cochrane Database of Systematic Reviews, 2007.
- Centers for Medicare & Medicaid Services (CMS). "Medicare Coverage of Carpal Tunnel Release Surgery." 2025.
Visual Guide Gallery





Walking Pad vs Treadmill
30-second comparison