Guide
Carpal Tunnel and Pregnancy: What to Know
By Dr. Laura Chen, Occupational Therapist & RSI Specialist · Updated 2026-03-10
This post contains affiliate links. We may earn a commission at no extra cost to you.
By Dr. Laura Chen, OT | Last updated: March 2026
Carpal tunnel syndrome during pregnancy is remarkably common, affecting between 31% and 62% of expecting mothers. The condition is caused by pregnancy-related fluid retention that compresses the median nerve in the wrist, leading to numbness, tingling, and pain — especially at night. The good news: most cases resolve within weeks of delivery, and safe, effective treatments exist to manage symptoms throughout pregnancy.
Table of Contents
- Why Pregnancy Causes Carpal Tunnel Syndrome
- Symptoms of Carpal Tunnel During Pregnancy
- When Does Pregnancy Carpal Tunnel Start?
- Risk Factors That Increase Your Chances
- Safe Treatments for Carpal Tunnel During Pregnancy
- Best Wrist Braces for Pregnancy Carpal Tunnel
- Exercises and Stretches for Relief
- When to See a Doctor
- Does Carpal Tunnel Go Away After Pregnancy?
- Carpal Tunnel and Breastfeeding
- Frequently Asked Questions
- Sources and Methodology
Why Pregnancy Causes Carpal Tunnel Syndrome
If you are pregnant and experiencing numbness, tingling, or pain in your hands, you are not imagining things. Carpal tunnel syndrome (CTS) during pregnancy is one of the most common musculoskeletal complaints expecting mothers face, and there is a clear physiological explanation for why it happens.
During pregnancy, your body retains significantly more fluid than normal. Blood volume increases by approximately 45% to support the growing baby, and hormonal changes — particularly rising levels of progesterone and relaxin — cause tissues throughout the body to swell and become more lax. This includes the tissues inside the carpal tunnel, a narrow passageway in your wrist formed by bones and a tough ligament called the transverse carpal ligament.
The carpal tunnel is already a tight space. Nine tendons and the median nerve all pass through it. When pregnancy-related edema causes the tissue inside this tunnel to swell, the median nerve gets compressed. This compression is what produces the characteristic numbness, tingling, and burning sensation in the thumb, index finger, middle finger, and half of the ring finger.
The problem tends to be worse at night because most people naturally bend their wrists while sleeping. A flexed wrist further narrows the carpal tunnel, which is why many pregnant women wake up at 2 a.m. shaking their hands to restore feeling.
A 2015 study published in the Journal of Hand Surgery (European Volume) found that pregnancy-related CTS is driven primarily by this fluid retention mechanism, which is distinct from the repetitive strain mechanism that typically causes CTS in the general population. This distinction matters because it means pregnancy carpal tunnel often resolves once the fluid retention subsides after delivery.
Understanding the cause helps you choose the right approach to treatment. Since the root issue is mechanical compression from swelling — not nerve damage from repetitive motion — conservative treatments like splinting, elevation, and gentle exercises are highly effective for most pregnant women.
Symptoms of Carpal Tunnel During Pregnancy
Recognizing the symptoms early allows you to start managing them before they interfere with sleep, daily tasks, and your overall comfort during pregnancy.
Primary Symptoms
The hallmark symptoms of carpal tunnel during pregnancy include:
- Numbness and tingling in the thumb, index, middle, and ring fingers. This is often described as a "pins and needles" sensation, similar to your hand falling asleep.
- Pain in the wrist and hand that can radiate up the forearm. Some women describe it as a burning or aching sensation.
- Nighttime worsening. Symptoms are almost always worse at night and in the early morning hours, often waking you from sleep.
- Weakness in grip strength. You may find it harder to grip objects, open jars, or hold a cup of coffee without fumbling.
- Swollen feeling in the fingers even when visible swelling is minimal. The fingers may feel stiff, clumsy, or "thick."
How Pregnancy Carpal Tunnel Differs From Regular CTS
There are several important distinctions. Pregnancy carpal tunnel tends to affect both hands simultaneously, while regular CTS is more commonly unilateral (one-sided). The onset is typically more gradual and tied to increasing fluid retention rather than a sudden injury or repetitive activity. And critically, pregnancy CTS has a much higher spontaneous resolution rate — most cases clear up on their own after delivery.
That said, the symptom experience can be just as disruptive. Many pregnant women report that nighttime hand numbness is one of the most frustrating aspects of their pregnancy, compounding the sleep difficulties that already come with the third trimester.
Symptoms to Take Seriously
While most pregnancy carpal tunnel is mild to moderate, certain symptoms warrant immediate medical attention:
- Constant numbness that does not come and go
- Muscle wasting at the base of the thumb (thenar atrophy)
- Dropping objects frequently due to hand weakness
- Symptoms that started before pregnancy and have gotten significantly worse
When Does Pregnancy Carpal Tunnel Start?
The timing of carpal tunnel symptoms during pregnancy follows a fairly predictable pattern that aligns with fluid retention changes.
Trimester-by-Trimester Breakdown
First trimester (weeks 1–12): Carpal tunnel symptoms are uncommon this early, though some women with pre-existing risk factors may notice mild tingling. Hormonal changes have begun, but fluid retention has not yet reached levels that compress the median nerve significantly.
Second trimester (weeks 13–27): This is when symptoms typically begin to appear, particularly toward the end of the second trimester around weeks 24 to 28. Blood volume is increasing rapidly, and many women start noticing mild nighttime hand numbness or morning stiffness.
Third trimester (weeks 28–40): Peak symptom severity. Fluid retention is at its highest, and the majority of women who develop pregnancy carpal tunnel will experience their worst symptoms during weeks 32 to 38. This is also when symptoms are most likely to start affecting daily activities like cooking, driving, and personal care.
A longitudinal study by Padua et al. (2010) published in Muscle & Nerve tracked pregnant women throughout gestation and found that 43% of participants developed electrophysiologically confirmed CTS by the third trimester, with symptom severity peaking at approximately 34 weeks.
Why Timing Matters
Knowing when symptoms typically peak helps you plan ahead. If you are entering your third trimester and have started noticing mild tingling, now is the time to get a wrist brace and begin preventive exercises rather than waiting until symptoms become severe enough to disrupt your sleep.
Risk Factors That Increase Your Chances
Not every pregnant woman develops carpal tunnel syndrome, and certain factors make some women more susceptible than others.
Established Risk Factors
Gestational diabetes and preeclampsia. Both conditions are associated with increased fluid retention, which directly increases pressure inside the carpal tunnel. Women with gestational diabetes have approximately twice the risk of developing CTS compared to those without it.
High BMI before pregnancy. Excess weight is associated with increased soft tissue volume within the carpal tunnel. Women who enter pregnancy with a BMI above 30 have a higher baseline risk.
Previous pregnancy carpal tunnel. If you experienced CTS during a previous pregnancy, you are significantly more likely to develop it again. The recurrence rate is estimated at 50% or higher.
Multiple pregnancies (twins, triplets). Carrying multiples causes greater fluid retention and hormonal changes, increasing CTS risk.
Age over 30. The carpal tunnel naturally narrows slightly with age, so older first-time mothers have a modestly increased risk.
Pre-existing conditions. Thyroid disorders, rheumatoid arthritis, and diabetes all increase baseline CTS risk, which pregnancy compounds.
Occupational Factors
Women who perform repetitive hand and wrist tasks — typing, assembly work, hairdressing, dental hygiene — have an elevated baseline risk of median nerve irritation. When pregnancy-related fluid retention is added to existing occupational strain, symptoms can develop earlier and more severely.
If you work at a desk, investing in an ergonomic mouse for carpal tunnel can reduce strain during those critical third-trimester weeks when your wrists are most vulnerable.
What You Cannot Control
Some risk factors are simply not modifiable. Your wrist anatomy (some people have naturally smaller carpal tunnels), genetic predisposition, and the hormonal profile of your specific pregnancy all play roles that you cannot change. The focus should be on managing modifiable factors and having a treatment plan ready.
Safe Treatments for Carpal Tunnel During Pregnancy
Managing carpal tunnel during pregnancy requires a different approach than typical CTS treatment because many standard interventions — certain medications, cortisone injections, and surgery — are either contraindicated or best deferred until after delivery.
Tier 1: First-Line Treatments (Start Here)
Wrist splinting. This is the gold standard treatment for pregnancy carpal tunnel and the single most effective intervention available. A neutral-position wrist splint worn at night prevents the wrist from flexing during sleep, which is when most compression occurs. Research consistently shows that nighttime splinting alone reduces symptoms in 60% to 80% of pregnant women.
Hand and wrist elevation. Keeping your hands elevated above heart level when possible helps reduce fluid accumulation in the wrists. Sleep with your arm propped on a pillow, and take breaks during the day to raise your hands.
Cold therapy. Applying an ice pack wrapped in a thin towel to your wrist for 10 to 15 minutes can reduce swelling and provide temporary pain relief. This is completely safe during pregnancy.
Gentle exercises and stretches. Specific wrist stretches and nerve gliding exercises can help reduce symptoms by improving blood flow and reducing adhesions around the median nerve. More on these below.
Tier 2: Additional Safe Interventions
Salt and fluid management. While you should not restrict fluid intake during pregnancy, reducing excess sodium can help minimize fluid retention. Discuss any dietary changes with your OB-GYN or midwife.
Ergonomic modifications. If you work at a computer, adjusting your keyboard height, using a wrist rest, and taking frequent breaks can reduce daytime symptoms. Your keyboard should be at elbow height, and your wrists should remain in a neutral position while typing. For a complete desk setup guide, see our article on best ergonomic keyboards for carpal tunnel.
Acetaminophen (Tylenol). For occasional pain relief, acetaminophen is generally considered safe during pregnancy when used as directed. It will not reduce the underlying swelling, but it can take the edge off pain that disrupts sleep. Always confirm with your healthcare provider first.
What to Avoid During Pregnancy
NSAIDs (ibuprofen, naproxen). These should be avoided during pregnancy, particularly in the third trimester, as they can affect fetal kidney function and close the ductus arteriosus prematurely.
Cortisone injections. While occasionally used in severe cases under specialist guidance, steroid injections are generally deferred during pregnancy unless symptoms are debilitating and not responding to conservative treatment.
Surgery. Carpal tunnel release surgery is almost never performed during pregnancy. Since most cases resolve postpartum, surgical intervention is reserved for the rare cases where severe nerve damage is occurring.
Best Wrist Braces for Pregnancy Carpal Tunnel
A wrist brace is the most effective tool in your carpal tunnel pregnancy toolkit. The right brace holds your wrist in a neutral position, prevents nighttime flexion, and reduces pressure on the median nerve — all without medication.
Here are five wrist braces that work well for pregnancy-related carpal tunnel, selected for comfort, adjustability (important as your body changes), and proper neutral positioning.
Check Pregnancy Wrist Braces on Amazon →

1. Mueller Green Fitted Wrist Brace
Best for: All-around pregnancy use (day and night)
Why it works: Contoured metal splint holds wrist at neutral. Breathable, antimicrobial fabric stays comfortable during warm pregnancy nights. Adjustable straps accommodate swelling changes.
Price: $12–$18
Check on Amazon →
2. Futuro Night Wrist Sleep Support
Best for: Nighttime-only use during pregnancy
Why it works: Cushioned palmar bead keeps wrist straight while sleeping. Fits either hand without adjustment. Open-finger design prevents overheating. One size fits most — no guessing with sizing.
Price: $10–$15
Check on Amazon →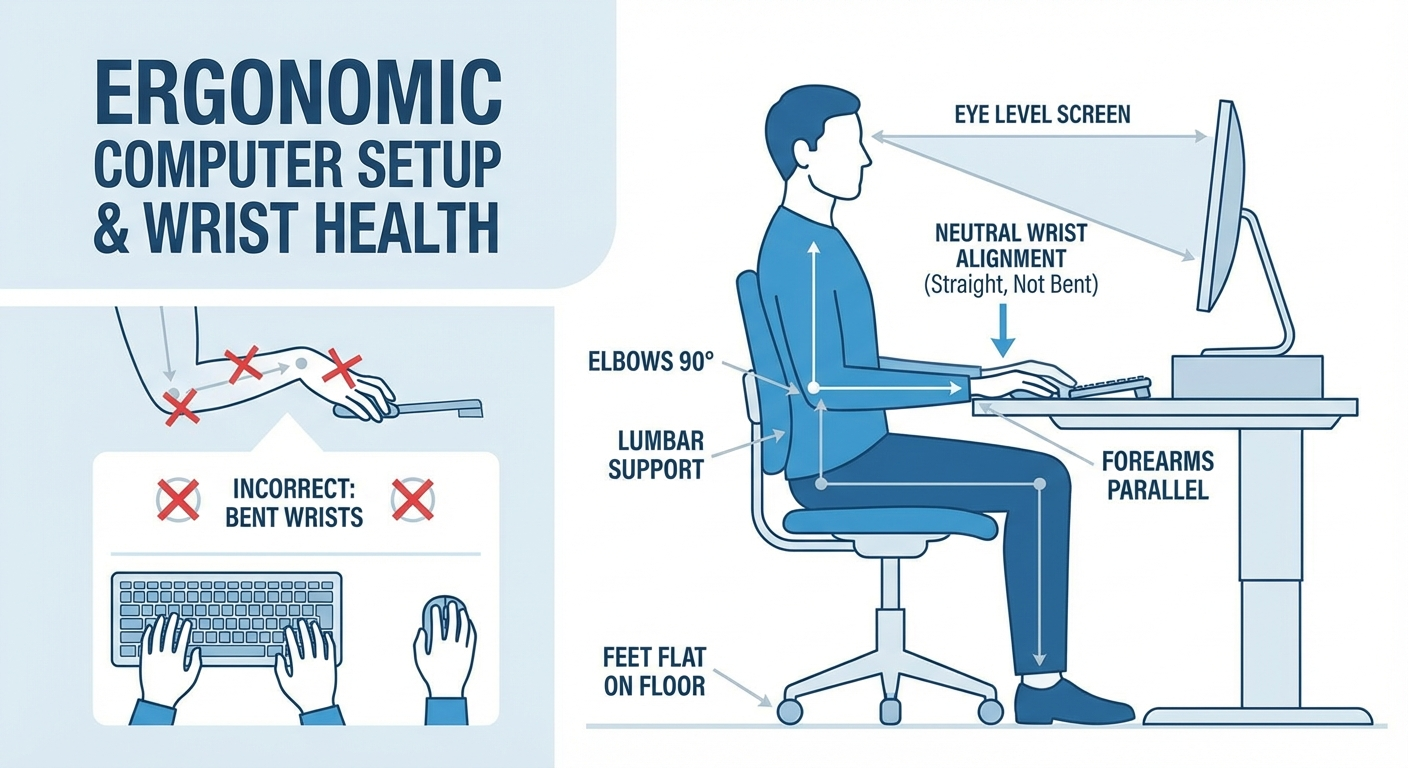
3. BraceAbility Carpal Tunnel Wrist Brace
Best for: Moderate to severe symptoms with swelling
Why it works: Extra-wide straps distribute pressure evenly over swollen wrists. Removable aluminum splint for customized fit. Comes in multiple sizes so you can size up if needed as pregnancy progresses.
Price: $20–$28
Check on Amazon →
4. Copper Compression Wrist Brace
Best for: Daytime wear while working or doing tasks
Why it works: Slim, low-profile design fits under clothing and allows typing. Copper-infused fabric provides mild compression without bulkiness. Breathable and moisture-wicking for comfort during pregnancy.
Price: $15–$22
Check on Amazon →
5. ComfyBrace Premium Night Wrist Splint
Best for: Sensitive skin and maximum comfort overnight
Why it works: Hypoallergenic inner lining is gentle on pregnancy-sensitive skin. Three adjustable straps allow precise fit as swelling fluctuates. Metal splint is removable for washing — important for hygiene during pregnancy.
Price: $14–$20
Check on Amazon →How to Choose the Right Brace for Pregnancy
The best brace for you depends on when and how you plan to wear it:
- Night only: Go with the Futuro Night Wrist Sleep Support or ComfyBrace. Both prioritize sleeping comfort over daytime functionality.
- Day and night: The Mueller Green Fitted Wrist Brace strikes the best balance. It is supportive enough for nighttime use but slim enough for daytime tasks.
- Severe symptoms with significant swelling: The BraceAbility offers the widest adjustability range, which is critical when your wrist circumference changes throughout the day.
- Desk work: The Copper Compression Brace has the lowest profile and allows the most finger mobility for typing and mouse use.
For a deep dive on brace selection, see our full guide on the best wrist braces for carpal tunnel.
Exercises and Stretches for Relief
Targeted exercises can significantly reduce carpal tunnel symptoms during pregnancy by improving blood flow to the median nerve, reducing adhesions, and gently mobilizing the nerve through the carpal tunnel.
1. Wrist Flexor Stretch
Extend your arm in front of you with the palm facing up. Use your other hand to gently pull your fingers back toward your body until you feel a mild stretch along the inside of your forearm. Hold for 15 to 20 seconds. Repeat three times per hand.
This stretch opens up the carpal tunnel entrance and relieves tension on the flexor tendons that share space with the median nerve.
2. Wrist Extensor Stretch
Extend your arm with the palm facing down. Gently press the back of your hand downward with your other hand until you feel a stretch along the top of your forearm. Hold for 15 to 20 seconds. Repeat three times per hand.
3. Median Nerve Glide
This is one of the most effective exercises for carpal tunnel during pregnancy. Start with your hand in a fist near your shoulder. Slowly straighten your fingers, then extend your wrist back, then straighten your arm, then gently turn your wrist so your palm faces the ceiling. Move smoothly through each position, holding each for 3 to 5 seconds. Complete five repetitions per hand.
Nerve glides help the median nerve slide more freely through the carpal tunnel, reducing irritation from adhesions.
4. Tendon Glide Sequence
Start with fingers straight. Make a hook fist (bend at the middle and end joints only). Then make a full fist. Then make a tabletop position (fingers straight, bent at the knuckles only). Return to straight. Repeat 10 times.
This sequence moves the tendons through their full range of motion inside the carpal tunnel, helping to reduce swelling around the nerve.
5. Wrist Circles
Extend your arms in front of you and slowly rotate your wrists in circles — 10 clockwise, then 10 counter-clockwise. This simple movement promotes blood flow and reduces stiffness.
6. Hand Elevation Pump
Raise both hands above your head and open and close your fists 10 times. This pumps fluid out of your wrists and hands through the venous system. Do this every hour when sitting for extended periods.
Exercise Routine for Pregnancy Carpal Tunnel
For best results, perform these exercises two to three times per day:
- Morning (before getting out of bed): Hand elevation pump + wrist circles
- Midday: Full sequence — flexor stretch, extensor stretch, nerve glide, tendon glide
- Evening (before putting on your night brace): Nerve glide + flexor stretch
For more detailed exercise instructions with step-by-step progressions, see our complete guide on carpal tunnel exercises.
When to See a Doctor
Most pregnancy carpal tunnel responds well to splinting and exercises, but there are situations where professional evaluation is necessary.
Red Flags That Require Medical Attention
Constant numbness. If the numbness in your fingers never goes away — not just at night but all day — this suggests significant nerve compression that may need more aggressive treatment.
Weakness causing functional problems. Dropping objects, being unable to button clothing, or difficulty gripping your steering wheel are signs that the motor branch of the median nerve is affected. This is more serious than sensory-only symptoms.
Visible muscle wasting. Look at the fleshy pad at the base of your thumb (the thenar eminence). If it appears flatter or smaller than the other hand, this indicates thenar atrophy from prolonged nerve compression.
Symptoms not improving after 2 to 3 weeks of splinting. If you have been wearing a wrist brace consistently at night for two to three weeks and see no improvement, your provider may want to consider additional interventions.
Symptoms that started before pregnancy. If you had carpal tunnel symptoms before becoming pregnant, the pregnancy may be worsening a pre-existing condition that may not fully resolve on its own after delivery.
What Your Doctor May Recommend
Your healthcare provider has several options depending on severity:
- Nerve conduction study. This electrodiagnostic test measures how well and how fast the median nerve conducts electrical signals. It confirms the diagnosis and helps grade severity.
- Occupational therapy referral. An OT can provide customized splinting, ergonomic recommendations, and a targeted exercise program.
- Corticosteroid injection. In severe cases where conservative treatment fails, a carefully considered steroid injection into the carpal tunnel can provide relief. This is generally considered safe during pregnancy when the benefits outweigh the risks, but it is not a first-line treatment.
- Postpartum surgical planning. If nerve conduction studies show severe compression during pregnancy, your doctor may plan for carpal tunnel release surgery after delivery if symptoms do not resolve.
Does Carpal Tunnel Go Away After Pregnancy?
This is the question every pregnant woman with carpal tunnel wants answered, and the news is mostly very good.
The Typical Postpartum Timeline
Weeks 1–2 after delivery: Many women notice improvement within the first two weeks as pregnancy-related fluid retention begins to resolve. The dramatic fluid loss that happens in the days following delivery can lead to noticeable symptom relief.
Weeks 2–6: Continued gradual improvement as hormonal levels normalize and residual edema clears. Most women report significant or complete resolution during this window.
Weeks 6–12: By three months postpartum, approximately 70% to 80% of women who had pregnancy-related carpal tunnel are symptom-free.
When It Persists
About 10% to 30% of women continue to experience some carpal tunnel symptoms beyond three months postpartum. Several factors predict a slower recovery:
- Breastfeeding. Hormonal changes associated with breastfeeding can maintain some degree of fluid retention, prolonging symptoms.
- Severe symptoms during pregnancy. Women who had severe nerve compression (confirmed by nerve conduction study) during pregnancy are more likely to have persistent symptoms.
- Pre-existing CTS risk factors. If you had risk factors before pregnancy — occupational strain, obesity, thyroid conditions — the pregnancy may have unmasked or accelerated an underlying problem that persists.
- Subsequent pregnancies. The carpal tunnel may already be sensitized from the previous pregnancy.
What to Do If Symptoms Persist
If your carpal tunnel symptoms have not resolved by three months postpartum, or if they are worsening rather than improving, request a nerve conduction study. This test will clarify whether there is ongoing nerve compression that might benefit from surgical release. The procedure (carpal tunnel release surgery) has a high success rate and a relatively straightforward recovery — see our guide on carpal tunnel surgery recovery for details.
Carpal Tunnel and Breastfeeding
Breastfeeding and carpal tunnel interact in two important ways that new mothers should understand.
Hormonal Effects
Breastfeeding maintains elevated levels of prolactin and can delay the complete normalization of pregnancy hormones. These hormonal changes can sustain some degree of fluid retention in the wrists, which means carpal tunnel symptoms may linger longer in breastfeeding mothers compared to those who formula feed. A study in the Journal of Obstetrics and Gynaecology Research found that breastfeeding mothers had a 1.5 to 2 times longer median time to symptom resolution.
Repetitive Strain From Breastfeeding Positions
The physical act of breastfeeding introduces a new source of wrist strain. Holding a baby's head during feeding, particularly while maintaining a C-hold grip on the breast or using a cross-cradle position, places sustained force on the wrist and forearm flexors. This repetitive strain can aggravate already-irritated carpal tunnel symptoms.
Tips for Breastfeeding With Carpal Tunnel
- Use a nursing pillow to support the baby's weight so your wrist does not have to.
- Alternate hold positions — try the football hold or side-lying position, which place less strain on the wrist.
- Continue wearing your wrist brace at night even after delivery until symptoms fully resolve.
- Do hand elevation pumps before and after feeding sessions.
- Take breaks and shake out your hands every 10 to 15 minutes during longer feeds.
Frequently Asked Questions
How common is carpal tunnel syndrome during pregnancy?
Carpal tunnel syndrome affects between 31% and 62% of pregnant women, most commonly developing during the second and third trimesters when fluid retention peaks. It is one of the most frequently reported musculoskeletal complaints in pregnancy, though many mild cases go unreported.
Does carpal tunnel from pregnancy go away after delivery?
Yes, in most cases pregnancy-related carpal tunnel resolves within 6 to 12 weeks after delivery as fluid retention decreases. However, about 10% to 30% of women may experience lingering symptoms for several months, especially if they are breastfeeding or had severe symptoms during pregnancy.
Is it safe to wear a wrist brace during pregnancy?
Yes, wrist braces are considered the safest and most effective first-line treatment for carpal tunnel during pregnancy. A neutral-position wrist splint worn at night keeps the wrist straight and reduces nerve compression without any medication or systemic effects. There are no risks to the baby.
Can carpal tunnel during pregnancy harm my baby?
No, carpal tunnel syndrome during pregnancy does not harm the baby. It is a condition affecting the mother's median nerve in the wrist and has no direct impact on fetal health, development, or delivery outcomes.
When should I see a doctor about pregnancy carpal tunnel?
See your doctor if you experience constant numbness that never improves, weakness that causes you to drop objects, visible muscle wasting at the base of your thumb, or symptoms that do not improve with splinting and home remedies after two to three weeks of consistent use.
What trimester does carpal tunnel usually start in pregnancy?
Carpal tunnel symptoms most commonly begin in the late second trimester or early third trimester, around weeks 28 to 34, when pregnancy-related fluid retention is at its highest. Some women notice earlier symptoms, particularly those with pre-existing risk factors like gestational diabetes or high BMI.
Can I take pain medication for carpal tunnel while pregnant?
Acetaminophen (Tylenol) is generally considered safe during pregnancy for occasional pain relief when used as directed. NSAIDs like ibuprofen should be avoided, especially in the third trimester, as they can affect fetal development. Always consult your OB-GYN before taking any medication during pregnancy.
Sources and Methodology
This article was researched and written by Dr. Laura Chen, an occupational therapist specializing in repetitive strain injuries, with specific attention to evidence-based management of carpal tunnel syndrome during pregnancy. All recommendations align with current clinical guidelines.
Sources cited:
-
Padua L, et al. "Carpal tunnel syndrome in pregnancy: multiperspective follow-up of untreated cases." Muscle & Nerve. 2010;42(2):145-151.
-
Ablove RH, Ablove TS. "Prevalence of carpal tunnel syndrome in pregnant women." Wisconsin Medical Journal. 2009;108(4):194-196.
-
Meems M, et al. "Prevalence, course and determinants of carpal tunnel syndrome symptoms during pregnancy: a prospective study." Journal of Hand Surgery (European Volume). 2015;40(8):838-844.
-
Stolp-Smith KA, et al. "Carpal tunnel syndrome in pregnancy: frequency, severity, and prognosis." Archives of Physical Medicine and Rehabilitation. 1998;79(10):1285-1287.
-
Mondelli M, et al. "Natural history of carpal tunnel syndrome during pregnancy." Acta Neurologica Scandinavica. 2007;115(2):91-95.
-
American College of Obstetricians and Gynecologists (ACOG). "Skin Conditions During Pregnancy" (FAQ 169). Revised 2020.
-
Osterman M, et al. "Carpal tunnel syndrome in pregnancy." Orthopedic Clinics of North America. 2012;43(4):515-520.
Dr. Laura Chen is a licensed occupational therapist with over 12 years of experience treating carpal tunnel syndrome and upper-extremity repetitive strain injuries. She holds a Doctorate in Occupational Therapy (OTD) and a Certified Hand Therapist (CHT) credential. Her work focuses on evidence-based, conservative management strategies for musculoskeletal conditions.



